
By Ginevra Liptan, MD
* Links may generate a commission for this site
Political trends and societal issues can have a huge impact on the practice of medicine, and lately nothing has been more controversial in medicine than the prescribing of opioids for pain. Opioids, or opiate-based pain medications, are chemically similar to opium (derived from the poppy plant) and include oxycodone, hydrocodone, and morphine.
Just as I was entering medical school in the late 1990s, there was a big push, led by chronic pain advocates and pharmaceutical companies, to improve the treatment of pain. Pain levels became the “5th vital sign,” and hospitals and medical offices were required to ask all patients to rate their pain level, in addition to checking blood pressure, pulse, height, and weight. This is why to this day, even if you are at the doctors office for a rash, they always asks you to rate your pain level on a 0-10 scale.
These efforts resulted in dramatic increases in opiate prescriptions, which nearly quadrupled between 1997 and 2002. Doctors also started getting sued for “under-treatment” of pain, leading to doctors prescribing even more opiates for pain to avoid lawsuits.
However, as prescriptions of opiates increased, so did abuse, diversion, and accidental deaths due to these medications. In 2007, deaths from unintentional drug overdoses killed almost 28,000 people in the U.S., and more than half of those deaths were from prescription opiate pain medications. In 2010 an article was published in the New England Journal of Medicine called “A Flood of Opioids, a Rising Tide of Deaths,” that described in detail the rising rates of accidental overdose as opiates were more heavily prescribed for chronic pain.
With mounting evidence of the dangers, over the past five years doctors started to prescribe less pain medications. State governments and health care companies also took action to lower the rate of opioid prescribing across the board. For example: In 2011, the state of Washington passed a law placing limits on the level of pain medications that primary care providers could legally prescribe without prior approval by a pain specialist.
Looking at the numbers of accidental deaths from opiates, it is hard to argue with the fact that they are dangerous medications that do need to be prescribed and monitored carefully. But I worry that the current trend toward limiting the ability of doctors to prescribe opiates will promote the under-treatment and stigmatization of those in chronic pain.
Instead, we should focus on programs that help doctors identify patients that are at high risk of accidental overdose from opiates, namely those that are abusing or misusing pain medications. Towards this end, many states now have successful prescription drug monitoring programs (PDMP), which provide reports on every controlled substance prescription a patient has filled in the state, so that doctors and pharmacies can quickly spot “doctor-shopping” and other signs of abuse or overuse of medications. The PDMP allows clinicians and pharmacists to monitor a patient’s prescription history for warning signs of potential drug abuse or safety issues, such as multiple prescribers or pharmacies, early refills, and high dosages.
Initial studies on the results of this type of programs are promising, with rates of abuse of opiate pain medications reducing between 2011 and 2013. In my experience, utilizing the PDMP has been incredibly helpful in allowing me to spot risky behavior in a few patients before it became dangerous, while I continue to prescribe much needed pain relief for the 99.9% of my patients that are using their medications safely and as prescribed.
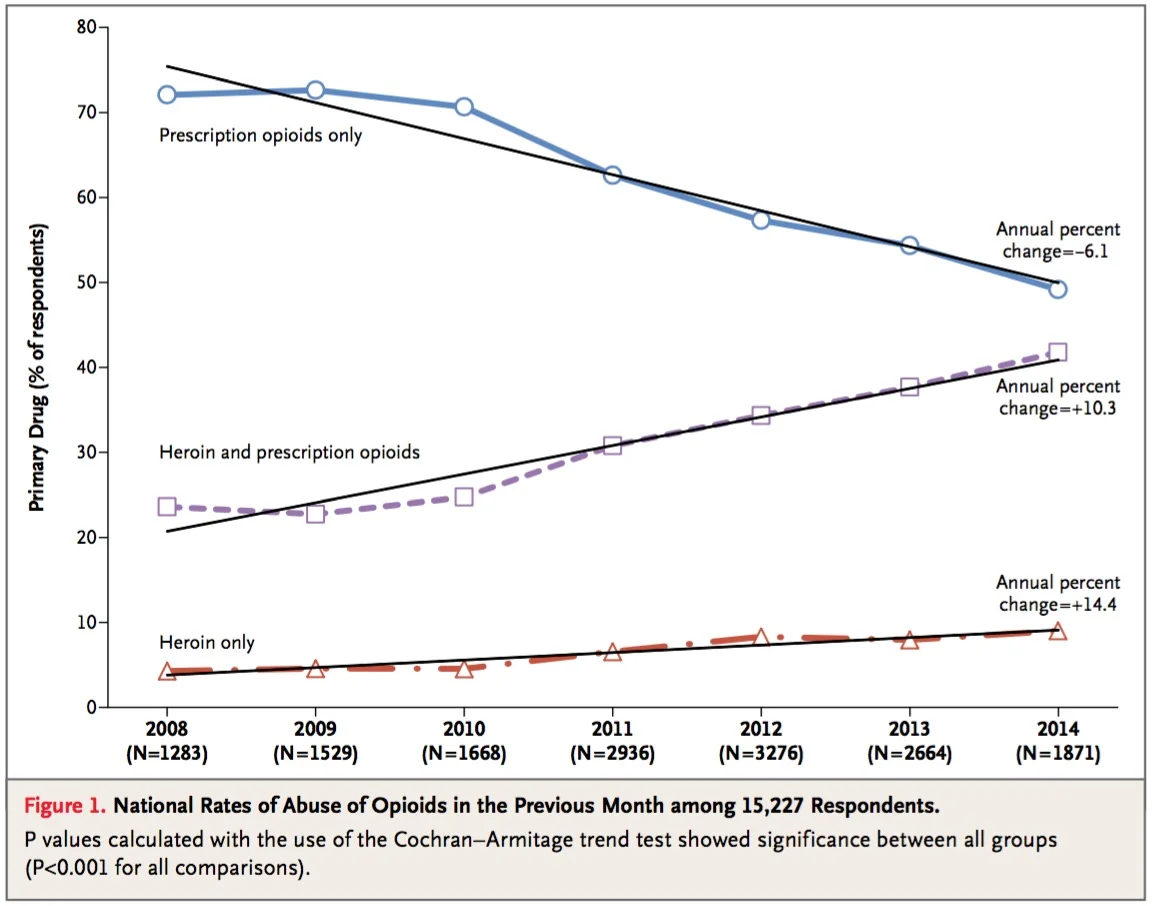
Click image to enlarge
Unfortunately as prescription opiate rates have gone down, heroin abuse has gone up. Heroin, a highly addictive drug of abuse, is also processed from opium and has some similar actions in the body as prescription pain medications. When people addicted to prescription opiate pain medications lose access, some start using heroin. This does not mean we should take away the right of everyone to access opiate pain medications. Instead the focus should be on trying to detect and treat addiction.
The historical parallels to prohibition are significant. Making alcohol illegal did not stop alcohol abuse, just as refusing to prescribe pain medications for those in chronic pain will not stop abuse of opiates. The problems of addiction and drug abuse run much deeper than that and need to be addressed more broadly in health care and society. In the meantime, we have to balance risk of societal harm with the right of individual patients to access effective pain relief.
Author Bio: Ginevra Liptan, MD, developed fibromyalgia while in medical school. She is a graduate of Tufts University School of Medicine and board-certified in internal medicine. Dr. Liptan is the founder and medical director of The Frida Center for Fibromyalgia and the author of The FibroManual: A Complete Fibromyalgia Treatment Guide For You...And Your Doctor and The Fibro Food Formula: A Real-Life Approach to Fibromyalgia Relief.